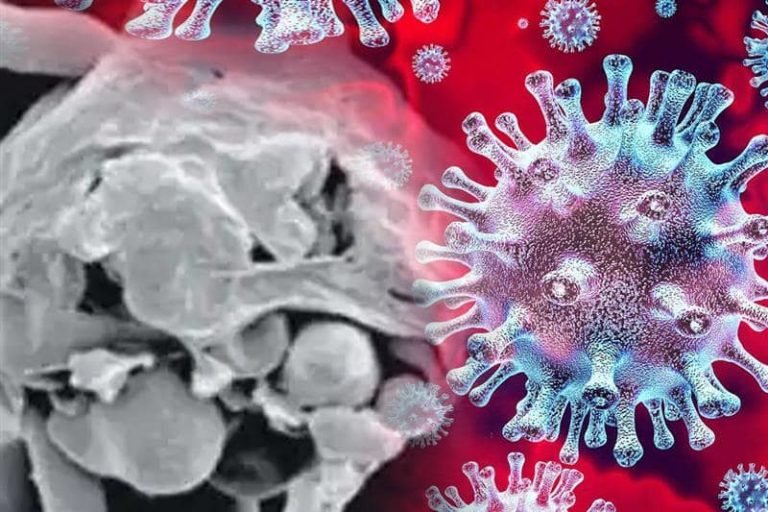
Read in Hindi: यहां जानिए ब्लैक फंगस और व्हाइट फंगस के कारण, लक्षण और इलाज
After four cases of white fungus were reported in Patna on Thursday, experts say that black fungus can cause more dangerous fungal infections. Meanwhile, India is witnessing an increase in cases of mucormycosis, or more commonly known as black fungi, as the country grapples with the deadly second wave of the COVID-19 epidemic.
The central government on Thursday urged the states and union territories to make mucormycosis or black fungus a notable disease under the Epidemic Diseases Act, stating that the infection is causing prolonged morbidity and COVID-19 in patients. Causing mortality. However, reports of white fungus cases have also raised concerns as the infection has been found to be more deadly than black fungi.
Dr. SN Singh, Head of the Department of Microbiology, said that the newly found fungal infection is prone to get oxygen support to the patients and it is reported to cause skin damage. If detected late, the infection could lead to death, he warned. The doctor appealed to cure COVID-19 and COVID-19 patients (who have tested negative) to take the white fungus seriously.
According to a Times of India report, both white and black fungal infections are caused by a mold of fungi called ‘mucormycites’ which are present in the environment.
White fungus
According to experts, infection of white fungus is more dangerous than black fungus because it has acute effect on lungs and other organs of the body. White fungus becomes more lethal as it spreads and causes great damage to vital organs. It can affect the brain, respiratory organs, digestive system, kidneys, nails or even private organs.
Black fungus
As cases of the black fungus, mucormycosis, are a matter of concern across the country, AIIMS director Randeep Guleria clarified that fungal infections are not new, but cases with COVID-19 have increased. Guleria said that ‘misuse’ of steroids is one of the major reasons behind black fungus cases.
“The disease (mucormycosis) can affect the face, infected nose, eye orbit, or brain, which can also cause vision loss. It can also spread to the lungs,” Guleria said, adding that people have infection control practices in hospitals K protocol should be followed. Guleria said, “It has been observed that secondary infections, fungal and bacteria, are leading to higher mortality.”
Who is more likely to be affected by white fungus?
According to a report by indianexpress.com, white fungi are more likely to infect people with low immunity. It can also occur when people come in contact with water or in a dirty environment containing mold. The disease is not contagious, but a person is said to be prone to infection because these molds can be easily taken in by a patient. The fungus can further spread to vital organs and cause complications.
People with low immunity, diabetes, cancer or those who use steroids regularly are at greater risk of getting infected with white fungus.
Who is more prone to black fungus?
Diabetic patients, COVID patients, and people on steroids are at greater risk of getting black fungal infections.
ICMR-an advisory by the Ministry of Health states that the major risk factors for the disease include uncontrolled diabetes mellitus, immunosuppression by steroids, prolonged stay in the ICU, malignancy and voriconazole therapy.
Symptoms and treatment of white fungus
Symptoms similar to COVID-19 are seen in patients with white fungal infection. Four white fungal cases reported at a hospital in Patna showed symptoms related to COVID, but did not test positive for COVID. In all cases, the lungs of the patients were found to be infected. Symptoms may also be similar to black fungus.
Since the white fungus affects the lungs and chest, it can cause cough, chest pain, shortness of breath. The infection may have inflammatory symptoms and may cause swelling, infection, persistent headaches, and pain.
While infection can be detected through X-rays and CT scans, patients are given anti-fungal medication to treat it. In cases reported in Patna, patients were given antifungal medicines and they recovered.
Symptoms and treatment of black fungus
Black fungus or mucormycosis is mainly affecting people recovering from COVID-19. Nose blackening or faded color, blurred or double vision, chest pain, shortness of breath and coughing due to infection. Mucormicosis mainly involves the sinus, the eye, and sometimes it may extend to the brain and may involve the nose. There have been few reports of pulmonary mucormycosis.
The Health Department of West Bengal has issued an advisory titled ‘Mukormicosis – If Uncured For – May Turn Fetal’, with warning signs of illness such as pain around the eyes or nose and redness, fever, headache, cough and vomiting. There is mention of suffering. Blood and ‘altered mental state’ – general changes in brain function such as confusion, amnesia, loss of alertness and
The advisory states that nasal congestion or closure, unilateral facial pain, numbness, darkening of the nose or palate, toothache, loosening of teeth, chest pain with blurred vision and respiratory symptoms. Deterioration is the suspected symptom of becoming infected. By mucormycosis.
The anti-fungal drug amphotericin-B is being used to treat cases of black fungus.
Important precautions to prevent black fungus:
According to an advisory issued by the Health Department of West Bengal, since people are vulnerable to infection due to exposure to fungal spores in the environment, people are exposed to rotting bread, fruits and vegetables in addition to soil, manure and excreta Has been warned to come. “When handling soil gardening, wear shoes, long trousers, long-sleeved shirts and gloves. People should maintain personal hygiene and are advised to scrub completely while bathing, ”said the consultant.
The disease can develop after the fungus enters the skin through cuts, burns or other types of skin trauma. The advisory states that the use of masks is essential, especially during visits to dusty construction sites. On the management of the disease, the Department of Health has recommended strict diabetes and diabetic ketoacidosis control as well as reducing steroids.
“Discontinue immunomodulating drugs and ingest normal saline before amphotericin B (an anti-fungal drug) infusion. To diagnose and to detect disease progression of patients clinically and with radio imaging Should be monitored,” the advisor read. In addition to mentioning the judicious use of steroids and antibiotics, Covid-19 discharges as well as monitored blood-sugar levels after routine examinations to find any warning signs.